Their genomes (the microbiome) endow us with physiologic capacities that we have not had to evolve on our own and thus are both a manifestation of who we are genetically and metabolically, and a reflection of our state of well-being. - Extending Our View of Self: the Human Gut Microbiome Initiative (HGMI) 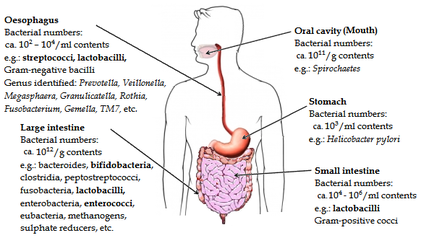 Microbes are everywhere: in the soil, in the water, in the air. They’re also in and on our bodies and in fact outnumber our own cells by about 10 to 1! Under our armpits, in between our toes, in our mouth, urogenital tract, and in our intestines…microbes like bacteria and fungi have a bad rap for causing food poisoning, body odor and infections, but let’s put those unpleasantries aside and talk about the incredible microbes living inside our gastrointestinal system that are inexplicably connected to our health and well-being. The human gut microbiome is estimated to consist of at least 10 trillion bacteria and archaea composed of about 1,100 prevalent species, with up to 400 species per individual. The gut microbial community has been called a “forgotten organ” with collective activity equal to organs as we know them. They interact primarily along our mucous membranes (skin that lines and protects the inside of our body: the inside of our nose and our urogenital, respiratory and digestive tracts), and one of their largest playgrounds is our digestive tract. In fact, cell densities in our colon are the highest recorded for any known ecosystem. While the details of how these microbes interact with our body are still incompletely understood and under the microscope, research is beginning to reveal how much they influence our digestion, metabolism, immune system, and even our mental health. Since our gastrointestinal friends cannot be cultured in the lab, much of the research that tells us how integral they are is done by comparing life with and without them. For example, microbe‐free animals are more susceptible to infection, have reduced digestive enzyme activity, increased inflammation and require a greater caloric intake to sustain a normal body weight. To cut a long story short, the gut microbiome:
This topic has consumed me the past few weeks and it’s taken much restraint to limit my research and ranting….The take-home point I want to share in this article is that our gut's microbiome is fantastically amazing and mysterious and its health ultimately affects our health….it’s a part of our body that we need to maintain harmony with. Now…how to do that? Well, below are some of the ways I've found through research. Of course this is not exhaustive as I am imperfect and the research is still underway. How do you maintain the health of your microbiome? Prebiotics & Probiotics Pre and Probiotocs have been getting a lot of publicity as of late and for good reason. I think of taking probiotics as the equivalent of restocking a pond with fish. Taking prebiotics, by contrast, is like nourishing and supporting the fish that are already in the pond. Probiotics are considered “good” bacteria, often found in live or cultured foods like foods like yogurt, kefir, buttermilk, sauerkraut, kimchi and other fermented and pickled versions of veggies, sourdough bread, miso (fermented barley or soy or rice), tempeh (fermented soy), and kombucha. Although more research is needed, some well-established effects of probiotics include:
Prebiotics are basically the foods that nourish our microbiome. I've already shared that I am all about fiber. Of the many reasons to love fiber is that it feeds our microbes! Unlike food rich in sugar and refined carbohydrates that break down in the small intestine, dietary fibers remain relatively intact all the way through the large intestine, providing a smorgasbord for our friendly microorganisms. A they feed, they, in turn, give off nutrients that nourish the cells that line our guts. Foods with prebiotics include chicory root, raw garlic, leeks, and onions, whole grains, fruits and vegetables and legumes. Prebiotics have been shown to:
Say no to artificial sweeteners Consumption of artificial sweeteners (saccharin, sucralose and aspartame) is considered safe, but emerging data should make us think again. Beyond their connection to weight gain (I will address this fascinating research in an upcoming post) a new study has found that that after 11 weeks, mice fed artificial sweeteners displayed glucose intolerance, a marker of risk for prediabetes and other metabolic disorders. This occurred via changes in the composition and function of the microbiome. In addition, preliminary data from the Personalized Nutrition Project has found that heavy consumers of artificial sweeteners have slightly elevated HbA1C levels (a long-term measure of blood sugar) compared with people who rarely or never consumed artificial sweeteners. I predict that this debate will intensify in the near future. Between now and then, let’s mitigate harm to our friendly gut microbiome and say no to diet beverages and avoid those colored packets when sweetening our coffee and tea. Also, read the ingredient list on your foods as they may be lurking in your gum, yogurt, flavored water, protein shakes, and powders, and cereal! More on controlling sugar cravings in blog posts to come. Be smart about antibiotic use Antibiotics deserve kudos for improving our health outcomes in the 20th century, but their usage also incurs risk. Beyond the rampant antibiotic resistance hurting our health care system at present, antibiotic use also hurts our gut’s microbiome. Unable to treat viral infections like the common cold or flu, antibiotics are commonly prescribed for bacterial infractions like skin, ear and bladder infections. They work by killing bacteria indiscriminately throughout the body. If you have an ear infection, for example, the antibiotic you take kills the good bacteria along with those causing you pain. Subsequently, you heal quickly but often incur antibiotic- associated disorders like inflammatory bowel disease, diarrhea and/or yeast infections. There is a current push for doctors to hold back on prescribing antibiotics and instead inspiring patients to manage symptoms with pain and fever reducers (like (Tylenol, Aspirin, and Ibuprofen) and decongestants. Talk with your doctor when battling an infection and learn about your options. In conclusion… It is becoming increasingly clear that our gut’s microbiome plays an important role in our health. An imbalanced microbiome can lead to the development of allergies, inflammatory bowel disease, obesity, diabetes…even cancer. All that being said, there doesn’t seem to be the “ideal” microbiome. Just as the ecosystems of forests, grasslands and coral reefs differ from place to place, so it is with microbiomes. Let’s keep our ears perked to the imminent research and recommendations and in the meantime, nourish our forgotten organ. ---- A fascinating side note is how we develop our microbiome. Its establishment begins immediately after birth and is influenced by the mode of delivery, infant diet (breast feeding is food for the microbiome too!), and medication. Babies born by Caesarean, a comparatively sterile procedure compared to a vaginal birth, do not acquire their mother’s microbes at birth. Their initial gut communities more closely resemble that of their mother’s (and father’s) skin, which is less than ideal and may account for higher rates of allergy, asthma and autoimmune problems in C-section babies. This is important to consider as rates of C-sections are up 50% since the mid 90’s with more than 1 in 3 infants being delivered by c-section in the U.S. For C-section deliveries research shows that infants being exposed to the vaginal microbiome of their mothers partially restores normal microbial colonization patterns to resemble vaginally delivered infants.
1 Comment
8/21/2018 03:01:21 am
This will totally help us with being more cautious with our health. To be honest, I didn't actually know almost all of the information that you have included here. Maintaining harmony with this microbiome is never really easy. But since I already have some idea about this, things will definitely be easier for me and I can even share this information with some of the people that I care about. Thank you so much for this and you know that I totally owe you for this.
Reply
Leave a Reply. |
AuthorHello and welcome! My name is Andrea Notch Mayzeles. I am a Certified Health Education Specialist, Mom, and Master of Public Health dedicated to the path of well-being. As a wellness professional I am committed to continued learning and am here to share research, recipes and musings on health, psychology, personal development, and parenting. I hope you enjoy! Categories
All
|

 RSS Feed
RSS Feed